β-adrenergic blockers are a class of pharmacologically diverse cardiovascular drugs recommended as first-line treatment for patients with hypertension and associated structural heart disease, as well as for those with angina and heart failure. Many intraclass differences exist, from pharmacokinetics and pharmacodynamics to ancillary actions such as intrinsic sympathomimetic activity, antiarrhythmic activity, α-1 adrenergic receptor blocking affinity, and direct vasodilation. Nebivolol's vasodilatory effects may lead to clinical outcomes with some unique characteristics. How does Nebivolol cause vasodilation? Nebivolol is a third-generation β1-selective, long-acting β-blocker that causes direct vasodilation through endothelium-dependent nitric oxide stimulation. Differences from other β-blockers may include improved endothelial function, enhanced muscle resistance artery perfusion, maintained exercise tolerance, and overall improved tolerability, side effects, and compliance. What is nebivolol used to treat? Nebivolol has been proven to be a clinically effective β-blocker for initial or adjunctive treatment of systemic hypertension, anti-anginal therapy, and treatment of patients with heart failure. Nebivolol uses in various treatments reflect its structural characteristics:
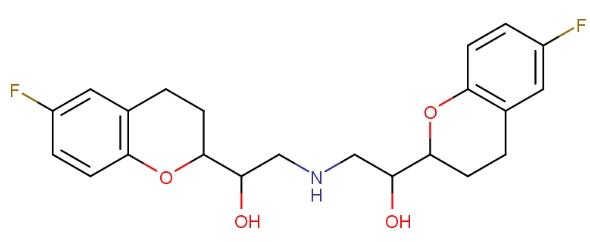
Why do doctors prescribe Nebivolol? Nebivolol is FDA-approved for treating hypertension. β-blockers are a class of drugs used to treat multiple conditions, including hypertension, angina, arrhythmias, anxiety, hyperthyroidism, migraine prevention, and essential tremor. The American College of Cardiology (ACC)/American Heart Association (AHA) guidelines recommend not using β-blockers as first-line treatment for hypertension but rather only for patients with comorbidities such as ischemic heart disease.
β-adrenergic antagonists can be categorized based on their mechanism of action: one type primarily blocks β-1 receptors in the myocardium, while the other blocks β-2 receptors in the lungs and smooth muscles, or both. Additionally, these drugs can be classified as either vasodilating or non-vasodilating depending on whether they possess vasodilatory properties. The U.S. Food and Drug Administration (FDA) has also approved a fixed-dose combination of Nebivolol with valsartan for the treatment of hypertension.
Nebivolol has received FDA approval for treating hypertension. Clinicians often prioritize prescribing β-adrenergic antagonists, ACE inhibitors, or ARBs for adults diagnosed with stable ischemic heart disease (SIHD) or those with both hypertension and a history of myocardial infarction or stable angina. Additionally, patients who have experienced a myocardial infarction or acute coronary syndrome are advised to continue guideline-directed medical therapy, including β-adrenergic antagonists, for at least three years as part of their long-term hypertension management.
Is nebivolol good for the heart? The 2021 European Society of Cardiology (ESC) heart failure guidelines recommend Nebivolol as an option for use in combination with first-line therapy. Nebivolol may also help treat microvascular angina. There is potential for Nebivolol to play a role in treating cancer therapy-related cardiac dysfunction (CTRCD), but further research is needed.

Adverse reactions to Nebivolol are typically related to the central nervous system (CNS). The most commonly reported adverse reaction is headache (6%-9%).
Nebivolol can be taken with or without food. It can be taken at any time of day. However, a prospective, randomized, double-blind, crossover study by Maria Czarina Acelajado et al. aimed to test the efficacy of taking Nebivolol in the morning versus at night in non-diabetic hypertensive patients. The study found that taking Nebivolol in the morning or at night significantly reduced 24-hour blood pressure parameters. Taking Nebivolol at night may have an advantage in reducing pre-awakening systolic blood pressure compared to taking it in the morning. However, follow the instructions of your healthcare provider.
Due to its electrophysiological properties, Nebivolol, like other β-blockers, increases the ventricular fibrillation threshold. This effect enables Nebivolol to reduce ventricular arrhythmias or drug-induced cardiomyopathy in various animal models. β-blockers are used to control irregular heartbeats in patients with atrial fibrillation (AF). By slowing the heart rate, symptoms caused by AF, particularly palpitations and fatigue, can often be improved. If you experience palpitations and are considering Nebivolol, ensure a comprehensive evaluation by a healthcare provider. They can determine the underlying cause of your palpitations and recommend the most appropriate treatment.
Nebivolol is primarily used to treat hypertension and heart failure. By selectively antagonizing β-1 receptors in the heart, it effectively manages both conditions by lowering heart rate and blood pressure. Nebivolol can also help alleviate symptoms associated with heart failure, improving patients' quality of life. While Nebivolol performs well in these treatments, each patient's situation is unique, so its use should be tailored according to a doctor's advice. To ensure optimal therapeutic outcomes and avoid potential side effects, consult a doctor before using Nebivolol and follow their professional guidance.
[1]https://www.ncbi.nlm.nih.gov/books/NBK551582/
[2]Priyadarshni S, Curry B H. Nebivolol[J]. 2019.
[3]https://www.webmd.com/drugs/2/drug-149866/nebivolol-oral/details
[4]https://www.sciencedirect.com/science/article/abs/pii/S1933171111002373
[5]https://www.sciencedirect.com/science/article/abs/pii/S0953620522002321
[6]https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4408822/
[7]https://www.bhf.org.uk/informationsupport/heart-matters-magazine/medical/drug-cabinet/beta-blockers
[8]https://www.sciencedirect.com/science/article/pii/S0828282X1400141X
 |
 |
 |