Miconazole nitrate, synthesized in 1969, is used to treat Candida vaginitis. It belongs to the imidazole class of antifungal drugs, chemically named 1-[2-(2,4-dichlorophenyl)-2-[(2,4-dichlorophenyl)methoxy]ethyl]-1H-imidazole nitrate, with the brand name Daktarin. This broad-spectrum antifungal drug is sensitive to both Candida and Gram-positive bacteria. Randomized trials show its efficacy in treating vaginal Candida infections can exceed 80%. The cream form is used for vulvar, male genital Candida infections, and skin Candida infections in neonates and infants. It can also be used during pregnancy after the first trimester under medical guidance.
Miconazole nitrate, with the English name Miconazole Nitrate, has a chemical formula of C18H14Cl4N2O·HNO3, CAS number 22832-87-7, and a molecular weight of 479.15. It appears as a white or off-white crystalline powder with little or no odor. It melts at 178-184°C, decomposing upon melting. It is slightly soluble in methanol, minimally soluble in chloroform or ethanol, and insoluble in water or ether. The structure of miconazole nitrate is as follows:
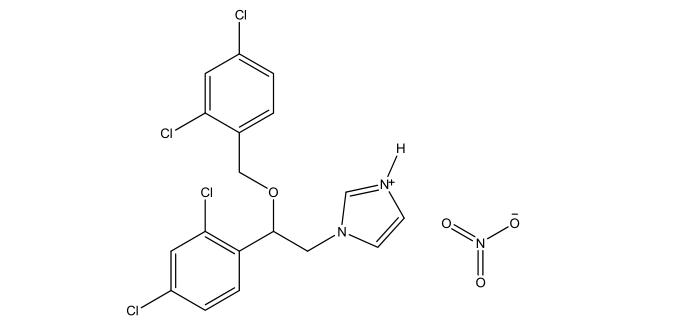
Miconazole nitrate is a broad-spectrum antifungal agent whose mechanism involves multiple cellular targets, collectively providing potent antifungal effects.
Targeting 14α-Demethylase: Miconazole nitrate specifically inhibits 14α-demethylase, a key enzyme in fungal cell membrane synthesis.
Disruption of Cell Membrane Structure: Inhibition of this enzyme impedes ergosterol synthesis, leading to the accumulation of toxic intermediates like lanosterol and disrupting membrane integrity.
Cell Death: Increased membrane permeability causes leakage of intracellular substances, ultimately leading to fungal cell death.
Binding to Phospholipids: Miconazole nitrate binds directly to phospholipids in the fungal cell membrane, further disrupting membrane structure and function.
Increased Membrane Permeability: This results in leakage of essential ions (such as potassium) and metabolites, accelerating cell death.
Oxidative Damage: Miconazole nitrate generates reactive oxygen species within fungal cells, causing oxidative damage to proteins, lipids, and DNA.
Synergistic Antifungal Effect: Oxidative stress, combined with other mechanisms, enhances the antifungal efficacy of miconazole nitrate.
Cytochrome P450 enzymes are involved in various metabolic processes within fungal cells. Inhibition of these enzymes disrupts essential metabolic pathways, weakening fungal survival.
In addition to its antifungal activity, miconazole nitrate exhibits inhibitory effects against some Gram-positive bacteria. This dual activity makes it an ideal choice for treating fungal and bacterial mixed infections.
Miconazole nitrate is widely used in current antifungal medications, such as Daktarin and Piconazole creams, where its primary ingredient is miconazole nitrate. This drug has a broad antifungal spectrum and is effective against several clinically important pathogenic fungi, including Candida albicans, Aspergillus species, Cryptococcus neoformans, Sporobolomyces, Coccidioides immitis, and Malassezia species. Additionally, miconazole nitrate demonstrates significant antibacterial activity against Gram-positive bacteria like Staphylococcus aureus, Streptococcus species, and Bacillus anthracis.
Clinically, miconazole nitrate is highly effective for various dermatophyte infections, such as tinea corporis, tinea cruris, and tinea pedis. Studies have reported a 1-week cure rate of 11.7%, with a total efficacy rate of 98.6% for tinea cruris, tinea corporis, and tinea cruris. The 2-week cure rate is 45.8%, with a total efficacy rate of 99.8%. The cure rate reaches 85.1% and total efficacy 99.7% one week after discontinuation. The fungal clearance rate is 93.9%. For Candida-induced vaginitis, miconazole nitrate shows superior efficacy compared to clotrimazole and nystatin. In studies comparing nystatin, clotrimazole, and miconazole nitrate for Candida vaginitis, the negative rates at week 6 are 60% and 67% for nystatin and clotrimazole, respectively, while miconazole nitrate achieves a 98% negative rate.
Miconazole nitrate eye drops act quickly at the infection site, useful for treating fungal keratitis. Clinical use of 0.1% miconazole nitrate eye drops has shown stable, broad-spectrum, low-toxicity, and good tissue penetration effects, with a 95% success rate in treating fungal keratitis in over 21 cases. Miconazole nitrate also exhibits good efficacy in treating fungal infections of the digestive system.
Common adverse reactions to miconazole nitrate include phlebitis, skin itching, nausea, fever, chills, rash, dizziness, and vomiting. Severe itching and rash require discontinuation of the drug. For nausea and vomiting, antihistamines or antiemetics can be used, and the medication should be taken away from meals if possible. The dosage may also be reduced. Miconazole nitrate may cause decreases in hematocrit, thrombocytopenia, and hyponatremia.
 |