Epinephrine Hydrochloride is widely used in clinical settings to handle emergencies such as cardiac arrest, severe asthma, and allergic reactions. This article explores the pharmacological effects, clinical applications, and potential adverse reactions of Epinephrine Hydrochloride to better understand the characteristics and uses of this important medication.
Epinephrine Hydrochloride, CAS: 329-63-5, with the molecular formula C9H14ClNO3, has a epinephrine hydrochloride molecular weight of 219.67. Epinephrine Hydrochloride is a sympathomimetic agent known for its fast onset, long-lasting effects, quick hemostasis, good efficacy, and minimal side effects. It stimulates both alpha and beta-adrenergic receptors, causing vasoconstriction, reducing intraoperative bleeding, and enhancing surgical efficiency. Additionally, it increases cardiac contractility and heart rate, boosting cardiac output. Recent reports indicate its effectiveness and safety in postoperative analgesia. Consequently, Epinephrine Hydrochloride is extensively used in modern medicine, particularly in surgeries such as facial plastic surgery, incision suturing, and tumor removal. However, common side effects such as arrhythmias, dizziness, headaches, and blood pressure abnormalities must be considered. Long-term use may lead to adverse outcomes like local tissue ischemia and necrosis.
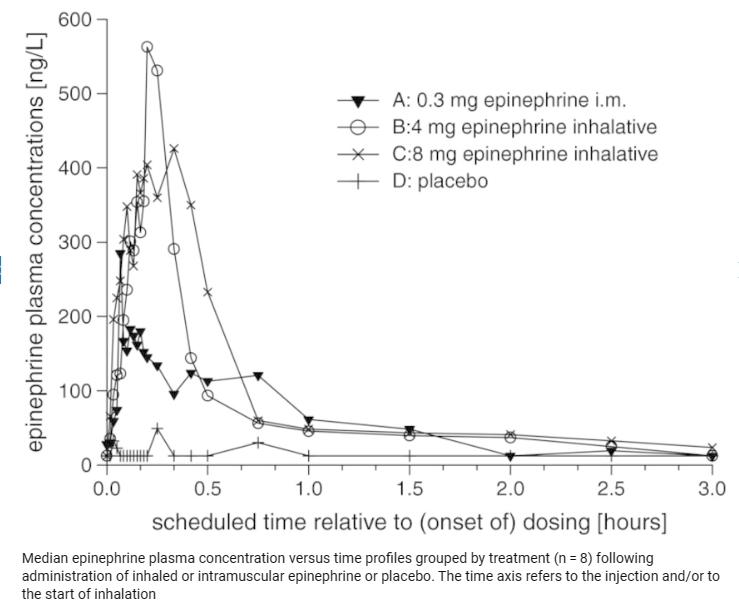
Epinephrine Hydrochloride has long been used to treat hypersensitivity reactions, with the epinephrine auto-injector (EpiPen) available in the U.S. since 1987. In recent decades, various new products, biosimilars, and formulations have been approved. On August 16, 2018, Teva Pharmaceuticals USA received approval to market generic epinephrine auto-injectors in 0.3 mg and 0.15 mg strengths. Administration routes for epinephrine include intravenous injection, inhalation, nebulization, intramuscular injection, and subcutaneous injection.
Epinephrine Hydrochloride injection is crucial for the emergency treatment of severe allergic reactions (anaphylaxis). Timely administration can be life-saving. Dosage depends on the severity of the allergic reaction, as well as the patient’s age and weight. It is essential to consult healthcare providers or follow specific guidelines for proper dosing.
Ensure the epinephrine auto-injector is not expired and the liquid inside is clear. Check the expiration date and for any signs of damage.
The preferred injection site is the outer thigh. Avoid areas covered by clothing or where bones are close to the skin.
Remove the safety cap. Firmly press the auto-injector against the thigh and push until a "click" is heard. Hold for a few seconds to ensure the full dose is delivered.
Safely dispose of the used injector according to local regulations. Do not attempt to re-cap the injector.
Even after administering epinephrine, immediate medical attention is necessary. Anaphylaxis requires thorough medical evaluation and treatment.
Familiarize yourself with the device and its instructions. Ensure the patient has no known contraindications to epinephrine. Always carry at least two doses of epinephrine, as one dose may not be sufficient.
Stay calm and focused. Administer promptly. Reassure the patient and have them lie down if possible.
What should you do immediately after giving an epinephrine injection? Monitor the patient closely for signs of improvement or worsening. Be prepared to perform CPR if necessary. Communicate with emergency medical services for prompt arrival.
Proper training in the administration of epinephrine is essential for everyone, especially caregivers, teachers, and individuals with known allergies. Being prepared and acting quickly can significantly impact the outcome of an anaphylactic reaction.
An overdose of epinephrine can lead to dangerous hypertension, cardiac issues, and even stroke, particularly in older adults.
Epinephrine may exacerbate existing heart problems, hypertension, or hyperthyroidism.
Epinephrine should only be used under a doctor’s prescription and with proper training in injection techniques.
Understand the dosage and potential side effects.
Disclose any pre-existing health conditions before using epinephrine.
Overdosing can cause serious complications. Follow the exact instructions for using an epinephrine auto-injector and seek immediate medical attention after use.
In high doses or in individuals with pre-existing heart conditions, epinephrine can increase the risk of arrhythmias or heart attacks.
Epinephrine typically causes temporary, manageable side effects.
Anxiety, nervousness, headaches, sweating, nausea, vomiting, paleness, dizziness, weakness, and tremors.
Most side effects will resolve on their own. Consult a doctor if symptoms are severe or persistent.
Store the epinephrine auto-injector in a cool, dry place away from direct sunlight and out of reach of children. Replace expired epinephrine promptly.
Epinephrine is crucial for emergency allergic reactions. However, be aware of potential risks and take safety precautions seriously. If you have concerns, consult your doctor.
Epinephrine Hydrochloride belongs to the therapeutic class of alpha and beta-adrenergic agonists (sympathomimetic agents). This classification system categorizes drugs based on their therapeutic effects. Epinephrine Hydrochloride mimics the effects of the sympathetic nervous system, including stimulating alpha and beta-adrenergic receptors throughout the body.
Epinephrine Hydrochloride is the hydrochloride salt of the naturally occurring sympathomimetic amine epinephrine. It has vasoconstrictive, ocular hypotensive, and bronchodilatory properties. By stimulating vascular alpha-adrenergic receptors, epinephrine causes vasoconstriction, increasing vascular resistance and blood pressure. When used in the conjunctiva, it binds to alpha-adrenergic receptors in the iris sphincter muscle, causing vasoconstriction, reducing aqueous humor production, and lowering intraocular pressure. Epinephrine increases the strength and rate of myocardial contractions through beta1-adrenergic receptor stimulation, and it relaxes bronchial smooth muscle, leading to bronchodilation.
Epinephrine Hydrochloride is an active sympathomimetic hormone from the adrenal medulla. It stimulates both alpha and beta-adrenergic systems, causing systemic vasoconstriction, gastrointestinal relaxation, cardiac stimulation, bronchodilation, and cerebral vasodilation. It is used for asthma, heart failure, and delaying the absorption of local anesthetics.
Epinephrine Hydrochloride is an important drug with the potential to play a critical role in cardiovascular emergency care and treatment. However, the use of Epinephrine Hydrochloride should be guided by medical advice and prescription instructions to ensure safe and effective treatment. If you have any questions or need further information about Epinephrine Hydrochloride or other related medications, it is recommended to consult a professional doctor or pharmacist for personalized health advice and guidance.
[1] https://www.drugs.com/sfx/epinephrine-side-effects.html
[2] https://pubchem.ncbi.nlm.nih.gov/compound/Epinephrine-Hydrochloride
[3] https://www.ncbi.nlm.nih.gov/books/NBK482160/
[4] https://go.drugbank.com/salts/DBSALT001484
[5] https://go.drugbank.com/drugs/DB00668
[6] Huang Jianbo. Clinical observation of the application of Epinephrine Hydrochloride in facial debridement and suturing surgery [J]. Northern Pharmacy, 2023, 20(07): 76-78.
 |
 |
 |